Acne Myths Busted – 10 Common Myths | Acne Skin Guide
The article aims to debunk 10 common myths surrounding acne, its causes, and treatments. It clarifies that foods like chocolate do not directly cause acne, poor hygiene is not the culprit, and stress is not the main trigger – dispelling myths around diet, cleanliness, and lifestyle factors. The article emphasizes that acne can occur at any age, not just during adolescence, and busts myths about quick-fix treatments like toothpaste or tanning.
It highlights that acne is not contagious, not just a cosmetic issue but a medical condition, and can affect all skin types and genders. While separating facts from fiction is crucial, the article acknowledges acne’s complexity, with individual triggers and responses. It stresses seeking professional dermatological guidance and reliable sources amidst misinformation. Ultimately, debunking myths promotes better understanding and effective acne management strategies.
#1 Recommended Acne Treatment | #2 Recommended Acne Treatment |
 |  |

Acne Myths Busted: Separating Fact from Fiction
Acne is one of the most common skin conditions, affecting millions of people worldwide. Despite its prevalence, numerous myths and misconceptions continue to circulate about its causes, triggers, and treatments. It’s time to separate fact from fiction and debunk these long-standing acne myths once and for all.
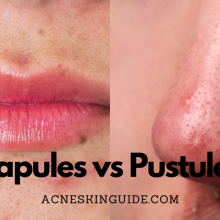
Myth #1: Chocolate and greasy foods cause acne
This is one of the most persistent myths about acne. While it’s true that a diet high in refined sugars and unhealthy fats can contribute to inflammation in the body, which may exacerbate acne, there is no direct causal link between specific foods like chocolate or french fries and acne breakouts. The relationship between diet and acne is complex, and moderation is key.
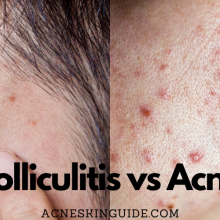
Myth #2: Acne is caused by poor hygiene
Contrary to popular belief, acne is not a result of poor hygiene or lack of cleanliness. In fact, over-scrubbing or using harsh cleansers can irritate the skin and worsen acne. Acne is primarily caused by a combination of hormonal factors, excess oil production, and bacterial overgrowth within the pores. While maintaining good hygiene is essential for overall skin health, it does not directly cause or prevent acne.
Myth #3: Stress is the main cause of acne
While stress can certainly aggravate existing acne, it is not the sole or primary cause. Acne is a complex condition involving hormonal imbalances, genetic predisposition, and other factors. However, managing stress levels is important, as chronic stress can increase inflammation and disrupt the body’s natural processes, potentially worsening acne.
Myth #4: Acne is just a teenage problem
This myth couldn’t be further from the truth. While acne is indeed prevalent during adolescence due to hormonal changes, it can affect people of all ages. Adult acne is a common phenomenon, often attributed to hormonal fluctuations, stress, and other lifestyle factors. It’s important to seek appropriate treatment regardless of age.
Myth #5: Toothpaste and harsh scrubbing can cure acne
This myth is not only false but also potentially harmful. Toothpaste contains ingredients that can dry out and irritate the skin, while harsh scrubbing can lead to over-exfoliation and inflammation. Effective acne treatment requires a gentle, consistent approach tailored to individual skin types and severity. Consult a dermatologist for professional guidance.
Myth #6: Acne is contagious
Acne is not a contagious condition. It is caused by internal factors such as hormones, genetics, and bacteria within the pores, not by external transmission. While it’s important to maintain good hygiene and avoid sharing personal items like towels or makeup, acne itself cannot be spread from person to person.
Myth #7: Tanning or sun exposure can clear up acne
This myth is not only false but also dangerous. While some individuals may experience temporary improvement due to the drying effects of UV rays, sun exposure can lead to long-term skin damage, premature aging, and an increased risk of skin cancer. Additionally, tanning can cause existing acne to become more inflamed and worsen scarring. Seeking professional acne treatments and using appropriate sun protection are recommended.
Myth #8: Acne is just a cosmetic issue
While acne may be primarily visible on the skin’s surface, it can have significant impacts on an individual’s self-esteem, mental health, and overall well-being. Acne is not just a cosmetic concern but a medical condition that deserves proper attention and treatment. Addressing the emotional and psychological effects of acne is just as important as treating the physical manifestations.
Myth #9: Acne only affects certain skin types or ethnicities
This myth perpetuates harmful stereotypes. Acne can affect individuals of all skin tones and ethnicities. While genetic factors may influence the prevalence or severity of acne in certain populations, it is a condition that transcends race or ethnicity.
Myth #10: Acne only affects females
Acne is a common misconception that only affects females, particularly during hormonal changes like puberty or menstruation. However, acne can affect individuals of any gender. While hormonal factors may play a role, both males and females can experience acne due to various underlying causes.
Conclusion
By debunking these persistent myths, individuals can gain a better understanding of acne and adopt more effective strategies for prevention and treatment. It’s important to seek professional advice from dermatologists, who can provide personalized guidance based on individual skin types, severity, and underlying causes.
However, it’s worth noting that while separating fact from fiction is crucial, some potential downsides and limitations exist. First, acne is a complex condition that may have unique triggers and responses for each individual. While general information can be helpful, it may not address specific cases or circumstances. Additionally, some acne myths persist due to personal experiences or anecdotal evidence, which can be challenging to overcome with scientific facts alone.
Moreover, the abundance of misinformation and conflicting advice on the internet and social media can make it difficult for individuals to discern reliable sources. It’s essential to consult reputable medical professionals and evidence-based resources when seeking information about acne and its management.
Despite these challenges, debunking acne myths and promoting accurate information is crucial for improving overall skin health and well-being. By separating fact from fiction, individuals can make informed decisions, adopt effective treatments, and avoid potentially harmful practices. Embracing a comprehensive and holistic approach to acne management, while seeking professional guidance, can lead to better outcomes and a deeper understanding of this common skin condition.
#1 Recommended Acne Treatment | #2 Recommended Acne Treatment |
 |  |
Summary and FAQs
Is it true that birth control pills can cause or worsen acne?
No, it’s a myth that birth control pills necessarily cause or worsen acne. In fact, certain birth control pills are often prescribed to help improve acne in women.
Here are some key points about birth control pills and acne:
1) Birth control pills help regulate hormones, specifically lowering androgen (male hormone) levels which contribute to acne formation.
2) Some women may experience temporary acne flare-ups when first starting birth control pills due to the initial hormone changes. However, after 2-3 months acne usually improves significantly.
3) The birth control pills that contain both estrogen and progestin tend to be most effective for improving acne.
4) Low-dose birth control pills with less estrogen may not provide the same acne-fighting benefits.
5) For some women with hormonally-influenced acne, birth control can help reduce breakouts by regulating the hormonal ups and downs during the menstrual cycle.
So in summary, while there may be an initial adjustment period, most dermatologists agree that birth control pills (when formulated appropriately) can be an effective part of an acne treatment regimen rather than a cause of worsening acne long-term.
Does popping or picking at pimples help get rid of acne?
No, popping or picking at pimples does not help get rid of acne and can actually make it worse. This is a dangerous myth that needs to be debunked.
Here are some key reasons why you should avoid popping or picking at pimples:
- It can lead to further inflammation and infection. Picking at pimples transfers dirt, debris and bacteria from your fingers into the pimple, allowing more bacteria to get inside.
- It increases the risk of acne scarring. The trauma from picking disrupts the skin’s healing process and damages the pimple further, leading to higher chances of permanent acne scars.
- It can cause pimples to spread. Popping releases bacteria and pus that can then spread across the face and body, causing more breakouts.
- It prolongs the pimple’s healing time. Picking repeatedly re-injures the pimple, restarting the inflammation cycle and delaying healing.
- It increases redness and swelling. The physical manipulation of squeezing pimples introduces more trauma and swelling to the area.
The proper way to care for a pimple is to gently wash the area, apply a spot treatment with benzoyl peroxide or salicylic acid, and avoid touching it. If a pimple needs draining, this should be done by a dermatologist using sterile techniques.
While tempting, popping or picking at pimples disrupts the skin’s natural healing and leads to worse acne – not an improvement. Breaking this myth is important for proper acne management.
Can drinking more water or staying hydrated clear up acne?
No, drinking more water or staying hydrated alone cannot clear up acne. This is a persistent myth that needs to be busted.
While proper hydration is important for overall health and can benefit skin health indirectly, there is no scientific evidence that drinking extra water has a direct impact on treating or preventing acne. Here are some key points debunking this myth:
- Acne is caused by factors like excess oil, clogged pores, bacteria, and hormones – not by lack of hydration or “toxins” that water can flush out.
- Skin hydration comes primarily from within the body via healthy oil production, not just by drinking water externally.
- Dehydration can potentially make acne appear slightly more pronounced as the skin becomes dull and dry, but it does not address the root causes of acne.
- Some studies have looked at the potential benefit of mineral waters on acne due to their anti-inflammatory properties, but regular drinking water showed no significant improvement.
- Dietary factors like excessive sugar, refined carbs and unhealthy fats may influence acne more than hydration levels.
While keeping the body well-hydrated has many overall health benefits, the specific claim that drinking more water clears acne is unfounded. Managing acne requires a multi-pronged approach including proper cleansing, medication when prescribed, hormone regulation and diet changes rather than simply increasing water intake alone.
Is it true that acne skips a generation?
No, the idea that acne skips a generation is a myth without scientific evidence to support it.
Here are some key points debunking the “acne skips a generation” myth:
- Acne has a strong genetic component, but it does not follow any pattern of skipping generations. If acne runs in a family, it can appear in multiple consecutive generations.
- The development of acne is influenced by the intricate interplay of genetics, hormones, and other biological factors – not by some mysterious generational skipping phenomenon.
- Acne can manifest differently in severity from one family member to another due to varying genetic makeup and environmental triggers, but it does not systematically skip a generation.
- Anecdotal claims of acne skipping a generation are likely coincidental rather than indicating any real biological pattern.
- Both teenage and adult acne can occur in the same family tree across multiple generations without following a skipping rule.
The predisposition to acne gets passed down based on the specific genes and hormonal factors inherited, not according to a generational skipping pattern. This myth likely arose from rare cases where a generational gap appeared by chance.
While genetics play a role, the development of acne depends on the complex interaction of many factors in each individual, not just the previous generation. Debunking this myth helps manage realistic expectations about acne risk in families.
Can using natural or organic skincare products cure acne?
No, using natural or organic skincare products alone cannot cure acne. This is a persistent myth that needs to be debunked.
While natural and organic products may be gentler and cause less irritation for some people, they are not inherently more effective at treating and curing acne than conventional, scientifically-proven acne treatments. Here are some key points:
- Acne is a medical condition that requires pharmaceutical-grade ingredients to treat effectively. Natural products rarely contain acne-fighting ingredients like benzoyl peroxide, retinoids, or antibiotics at therapeutic levels.
- The terms “natural” and “organic” are loosely regulated and don’t necessarily mean the products are safer or more effective, especially for treating acne.
- Some natural ingredients like tea tree oil have antibacterial properties but require very high concentrations to work against acne, which can irritate skin.
- Dietary supplements and detox claims around natural products “curing” acne from the inside-out are not backed by scientific evidence.
- Dermatologists emphasize that while natural products are fine for basic cleansing, treating acne requires medical-grade treatments prescribed based on severity.
The myth likley persists due to the marketing of natural products as “gentler” alternatives and people hoping for an easy, natural cure. However, effective acne treatment requires science-backed medications, sometimes combined with natural product routines.
While exploring natural options, it’s important to have realistic expectations and not forego proven acne treatments prescribed by a dermatologist in the process. Severe, stubborn acne requires medical intervention beyond natural products alone.